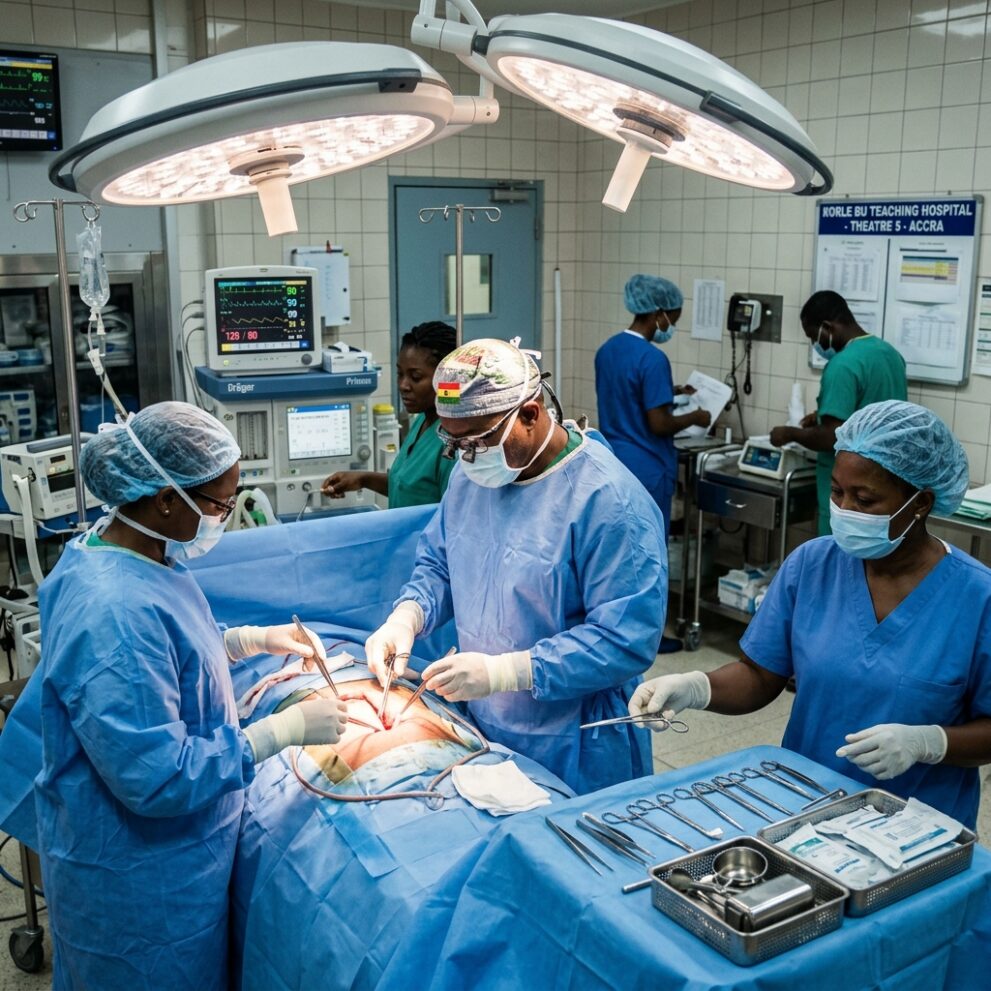
The NCDs are rising at an alarming rate in this country
Honorable Kwabena Mintah Akandoh
Ghana stands at a critical public health crossroads. Non-communicable diseases, commonly called NCDs, are no longer a distant threat; they are now a dominant cause of mortality across the country. Recent government statements reveal that about 42 to 45 percent of deaths in Ghana are now attributable to NCDs, a dramatic shift that demands urgent national attention, strategic prevention, and community-level action. This surge in chronic conditions—chiefly hypertension, diabetes, and cardiovascular disease—creates a dual burden for Ghana’s health system: the persistent challenge of
infectious diseases combined with a fast-growing wave of long-term illnesses that silently erode lives, livelihoods, and economic stability. The scale of the problem means that traditional clinic-centered approaches are insufficient; the solution must be proactive, community-driven, and built around early detection and prevention. That statement captures the reality facing families and health workers across Ghana: many people live with undiagnosed conditions until complications force emergency care. Early detection is not optional—it is the single most effective lever to reduce premature deaths and long-term disability.
Free primary healthcare and nationwide screening are central to the government’s response. By expanding access to basic services and taking screening into communities and homes, health authorities aim to identify high blood pressure, elevated blood sugar, and other risk markers before they progress to life-threatening stages. This approach is designed to remove cost barriers and to meet people where they live, work, and worship—because convenience and trust determine whether screening programs succeed.
Prevention saves lives and money. Investing in community screening, health education, and early treatment reduces hospital admissions, prevents costly complications, and preserves workforce productivity. Practical, evidence-based interventions—such as routine blood pressure checks, blood glucose testing, tobacco cessation support, and community nutrition counseling—deliver measurable returns when scaled across districts and regions. These interventions must be paired with robust referral pathways so that people identified with risk factors receive timely follow-up care.
A successful national strategy requires three interlocking pillars: access, awareness, and continuity. Access means free or affordable primary care services and mobile screening units that reach rural and peri-urban populations. Awareness means culturally tailored campaigns that explain risk factors, symptoms, and the benefits of early testing. Continuity means reliable systems for follow-up, medication supply, and long-term management—so a diagnosis becomes the start of care, not a sentence to repeated crises. The government’s plan to integrate screening into free primary healthcare is a step in this direction, but implementation must be rapid, well-resourced, and data-driven.
Data and monitoring are essential. National screening campaigns should be accompanied by a centralized data system that tracks screening coverage, diagnoses, treatment initiation, and outcomes. Real-time data enables targeted outreach to underserved areas, identifies supply chain gaps for essential medicines, and measures program impact. Transparent reporting builds public trust and helps donors and partners align resources where they are most needed.
Health financing must be sustainable. Free primary healthcare initiatives must be matched with predictable funding for medicines, diagnostics, and community health worker programs. Public-private partnerships can expand capacity, but government stewardship is critical to ensure equity and quality. Insurance schemes and social protection programs should explicitly cover chronic disease management to prevent catastrophic out-of-pocket spending that pushes families into poverty.
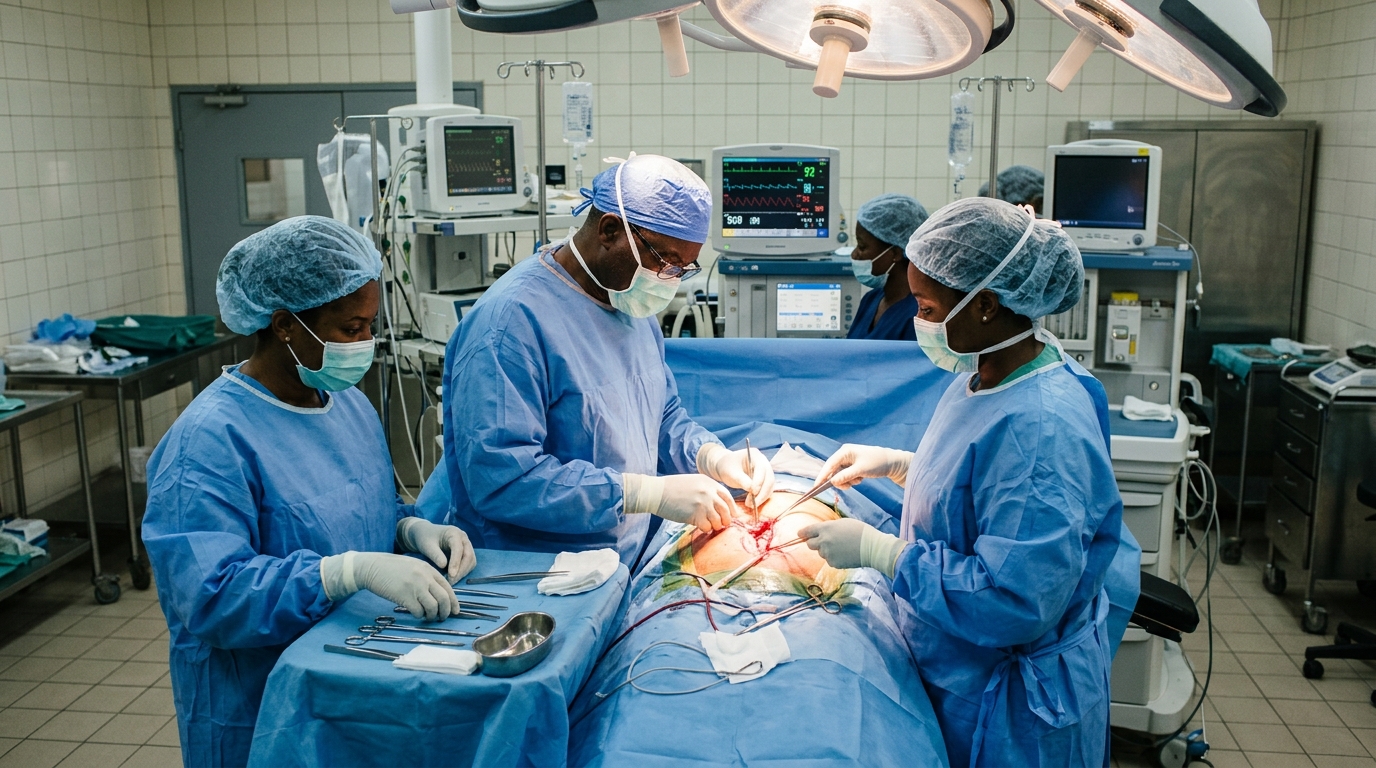
Clinicians and frontline health workers need training and tools to manage NCDs effectively at the primary care level. Task-shifting—empowering nurses and community health officers to perform routine screening and follow-up—can expand reach without compromising quality. Standardized treatment protocols, continuous professional development, and supportive supervision ensure that patients receive evidence-based care close to home.
The human stories behind the statistics matter. Families lose breadwinners to sudden heart attacks, workers are sidelined by complications of untreated diabetes, and children bear the economic and emotional burden when parents fall ill. Framing NCDs as a national development issue—not just a health problem—mobilizes broader support from finance ministries, employers, and international partners. When leaders recognize that healthier populations are more productive and resilient, investments in prevention become a national priority.
What can individuals do right now? Start with simple, high-impact steps: get a blood pressure check, test blood sugar if you are over 40 or have a family history, reduce salt and sugar intake, increase daily physical activity, avoid tobacco, and seek medical advice early if you notice warning signs. Community screening events are an ideal opportunity to take action—participation can mean the difference between early treatment and a life-threatening emergency.
The scale of the challenge is daunting, but the path forward is clear: detect early, treat promptly, and prevent relentlessly. Ghana’s renewed focus on free primary healthcare and community screening is a promising foundation. To turn policy into impact, the program must be comprehensive, well-funded, and sustained over years—not months. The cost of inaction is measured in lives lost, families disrupted, and economic setbacks that could have been avoided.
In the words of the Health Minister, the country must “move into the homes of Ghanaians to do simple screening.” That simple, community-centered approach—backed by strong policy, financing, and data—can reverse the trend of rising NCD deaths and protect future generations. The time to act is now: every screening, every counseling session, and every medication supplied is a step toward a healthier Ghana.